HomeDivisionsHeart DiseaseCoronary Artery Disease
The heart is a fist-sized muscle that beats about 70 times per minute and pumps oxygen-rich blood around the body in a process called circulation.
After leaving the heart, blood travels to the lungs where it collects oxygen.
This oxygen-rich blood from the lungs then returns to the heart where it is pumped to organs throughout the body through blood vessel called arteries.
The blood returns to the heart through the veins — a different type of blood vessels — and is again pumped to the lungs.
Coronary arteries are the heart’s own network of blood vessels that are located on the surface of the heart.
Coronary arteries are critical for the proper functioning of the heart because they supply the heart muscle with oxygen.
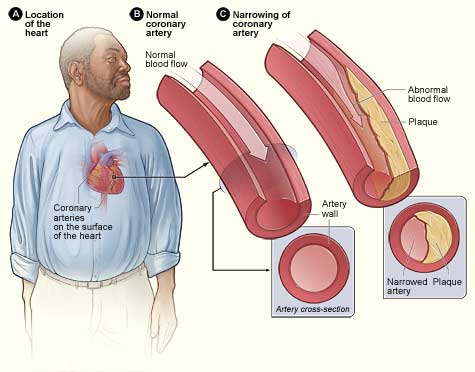 So, what is coronary artery disease? Coronary artery disease (CAD), also called coronary heart disease (CHD), or simply, heart disease, is a narrowing of the blood vessels (coronary arteries) that supply oxygen and blood to the heart.
So, what is coronary artery disease? Coronary artery disease (CAD), also called coronary heart disease (CHD), or simply, heart disease, is a narrowing of the blood vessels (coronary arteries) that supply oxygen and blood to the heart.
It is the most common type of heart disease. Coronary artery disease and its complications are the leading cause of death for males and females in the U.S., affecting more than 16 million Americans. In 2008, 405,309 individuals in the U.S. died from coronary artery disease.
Although the terms coronary artery disease are often used interchangeably, coronary heart disease is technically a result of coronary artery disease.
In coronary artery disease, the arteries narrow because of the accumulation of plaque, a fatty substance composed of cholesterol, a blood-clotting material called fibrin, and other compounds, on the artery walls.
When the inner wall of an artery is damaged, these fatty deposits build up at the injured sites in a process called atherosclerosis.
The buildup of plaque limits the flow of blood to the heart, causing a reduction in oxygen.
Atherosclerosis can lead to a condition called ischemia, or oxygen starvation of the tissues.
Cardiac ischemia, or oxygen-deprivation of heart muscle, develops when the arteries have become too narrow to permit oxygen-rich blood to reach the heart.
Ischemia is often experienced during exercise or exertion, eating, excitement or stress, or exposure to cold.
Atherosclerosis, the major defect in coronary artery disease, is closely associated with oxygen-starvation of the heart.
Atherosclerosis increases the risk for angina pectoris (chest pain), shortness of breath, heart attack and stroke.
There are 2 types of plaque: hard and soft that contribute to blockage of the arteries. Hard plaque can cause chest pain (angina) by diminishing, slowing, or even stopping the flow of oxygen-rich blood to the heart muscle.
If atherosclerotic plaques totally obstruct the coronary arteries, a heart attack may occur.
Soft or vulnerable plaque can lead to the formation of a blood clot, which can abruptly cut off the blood supply to the heart and trigger heart attack.
A blood clot that restricts the heart’s blood supply can cause permanent heart damage.
Coronary artery disease starts in childhood followed by a progressive, lifelong deposit of cholesterol-laden plaque.
Over time, the plaques release chemicals that help to heal the inflamed, blood vessel walls but at the same time make the inner walls of the blood vessel sticky.
Coronary artery disease weakens the normally smooth and elastic arteries, causing them to become narrow and rigid.
Without adequate oxygen and vital nutrients delivered to the heart, the damaged or diseased heart muscle in coronary artery disease can lead to serious complications.
SYMPTOMS OF CAD
Signs and symptoms of coronary artery disease due the buildup of plaque in the coronary arteries include:
- Chest pain (angina pectoris)
Chest pain, the most common symptom of coronary artery disease, is experienced as a heaviness, discomfort, or tightness pressure, aching, burning, numbness, fullness, squeezing or painful feeling. It is felt in the area of the heart muscle receiving inadequate blood oxygen flow. Angina may be mistaken for indigestion or heartburn. While angina usually occurs in the chest, it also may be felt in the left shoulder, arms, neck, back, or jaw. The pain often radiates to the neck, jaw, arms, shoulders, throat, back, or sometimes the teeth. Angina may be accompanied by symptoms of indigestion, heartburn, weakness, sweating, nausea, cramping, and shortness of breath. There are several types of angina:- Stable (chronic) angina is predictable and usually lasts a short period of time. It may feel like gas or indigestion. It occurs when the heart has to pump harder to move blood, as during strenuous physical activity. Symptoms subside with rest or medication.
- Unstable angina, often triggered by blood clots, occurs at rest and is unpredictable. Symptoms last longer than in chronic angina and may worsen over time.
- Variant angina is usually severe and occurs at rest when an artery has a spasm, causing it to narrow and limit the blood supply to the heart. Exposure to cold, stress, medicines, smoking, or cocaine use can lead to variant angina.
-
- Congestive Heart Failure
Congestive heart failure may develop if some areas of the heart are chronically deprived of oxygen and nutrients due to reduced blood flow, or if the heart has been damaged by a heart attack. If these conditions occur, then the heart may become too weak to pump sufficient blood to meet the body’s needs. This condition is called heart failure. - Abnormal Heart Rhythm (Arrhythmia)
Inadequate blood supply to the heart or damage to heart tissue can interfere with the heart’s electrical impulses, resulting in abnormal heart rhythms. - Shortness of Breath
Shortness of breath may occur if the heart and/or other body organs are not receiving adequate oxygen-rich blood from the heart. The patient may start panting and possibly become extremely fatigued with exertion. - Palpitations (irregular heart beats, skipped beats, or a “flip-flop” feeling in the chest)
- Faster Heartbeat
- Weakness or Dizziness
- Nausea
- Sweating
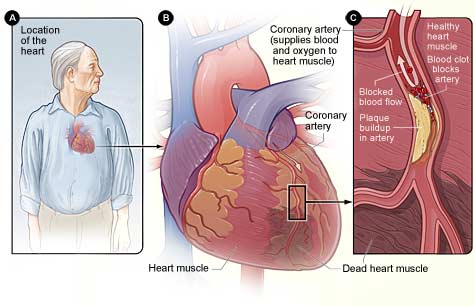
- Heart Attack (Myocardial Infarction)
If a cholesterol plaque ruptures and causes the formation of a blood clot, one of the coronary arteries may become completely obstructed, triggering a heart attack. Insufficient blood flow to the heart may damage the heart muscle. The extent of damage depends partly on how quickly the patient receives treatment. Other terms for heart attack are cardiac infarction and coronary thrombosis.Classic signs and symptoms of a heart attack include crushing pressure in the chest and pain in the shoulder or arm, sometimes with shortness of breath and sweating. Women tend to have less typical signs and symptoms of a heart attack, and instead may experience nausea and back or jaw pain. In some cases, there are no apparent signs or symptoms during a heart attack.
- Congestive Heart Failure
 Signs of a heart attack
Signs of a heart attack
-
- Chest discomfort, mild pain
- Coughing
- Crushing chest pain
- Dizziness
- Dyspnea (shortness of breath)
- Face appears gray
- A terrifying feeling that a person’s life is coming to its end
- Generally awful feeling
- Nausea
- Restlessness
- Clammy and sweaty in various parts of the body
- Vomiting
Causes of Coronary Artery Disease
Damage to the coronary arterial walls and the shrinking diameter of the blood vessels that lead to coronary artery disease is caused by:
• Smoking
• High blood pressure
• High cholesterol levels (lipoproteins)
• Diabetes
• Radiation therapy to the chest, as used to treat some types of cancer
Risk Factors of Coronary Artery Disease
Some of the risk factors overlap with the causes of coronary artery disease. Risk factors for coronary artery disease include:
• High blood pressure
Uncontrolled high blood pressure can lead to hardening and thickening of the arteries that in turn narrows the blood vessels. This can reduce blood flow to the heart.
High blood cholesterol levels
• Low-density lipoprotein (LDL)
Elevated levels of cholesterol in the blood increase the risk of atherosclerosis or plaques forming in the coronary arteries. Low-density lipoprotein (LDL), commonly called “bad” cholesterol, leads to increased cholesterol levels. Lipoprotein forms when an LDL particle attaches to a specific protein. This type of lipoprotein may disrupt the body’s ability to dissolve blood clots. Elevated levels of this particular lipoprotein may increase the risk of cardiovascular disease, including coronary artery disease and heart attack.
• High-density lipoprotein (HDL)
a low level of another type of lipoprotein called high-density lipoprotein (HDL) (“good” cholesterol) also can lead to atherosclerosis.
• Diabetes
Diabetes is linked with an increased risk of coronary artery disease. Risk factors such as obesity and high blood pressure contribute to both diabetes and coronary artery disease.
• Obesity
Excess weight exacerbates other risk factors for coronary artery disease.
• Older age
The risk of damaged and narrowed arteries increases with age.
• Sex
Men overall have a higher risk of coronary artery disease than women. Men older than 45 years of age are at risk. However, the risk for women rises after menopause.
• Family History
A family history of heart disease is associated with an increased risk of coronary artery disease, particularly if a close relative developed heart disease at an early age. The risk is greatest if a person’s father or a brother developed coronary artery disease before age 55, or if his or her mother or a sister was diagnosed with this condition before age 65.
• Smoking
Smokers have a higher risk for coronary artery disease because nicotine narrows the blood vessels, and carbon monoxide can damage the inner lining, making them susceptible to atherosclerosis. Women who smoke at least 20 cigarettes a day are 6 times more likely to have a heart attack than women who have never smoked. Men who smoke have 3 times the incidence of coronary artery disease as men who are nonsmokers.
• Physical Inactivity
Lack of exercise or physical activity is associated with coronary artery disease as well as some of its risk factors such as obesity and high-density lipoprotein (HDL) (“good” cholesterol).
• High Stress Levels
Unmanaged stress may damage the arteries and also worsen other risk factors for coronary artery disease.
• Risk Factor Clusters
Certain risk factors that cluster, or occur together, further increase the risk of coronary artery disease. Metabolic syndrome — a combination of conditions that includes elevated blood pressure, high triglycerides, high insulin levels and excess body fat around the waist — raises the risk of coronary artery disease.
Other possible factors implicated in the onset of CAD include:
• Sleep apnea
This condition causes a person to repeatedly stop and start breathing while sleeping. Sleep apnea results in an abrupt drop in blood oxygen levels that increase blood pressure and strain the cardiovascular system, potentially triggering coronary artery disease.
• C-reactive protein
C-reactive protein (CRP) is a protein normally found in the body that occurs in increased amounts when inflammation is present. High CRP levels may be a risk factor for heart disease. It appears that CRP protein levels increase as coronary arteries narrow.
• Homocysteine
Homocysteine is an amino acid used by the body to make protein and to build and maintain tissue. Elevated levels of homocysteine may increase the risk of coronary artery disease.
• Fibrinogen
Fibrinogen is a protein in the blood involved in blood clotting. However, excessive fibrinogen may increase clumping of platelets, a type of blood cell responsible for clotting. The formation of a clot in an artery may trigger a heart attack or stroke. Fibrinogen may also reveal inflammation often associated with atherosclerosis.
Diagnosis of Coronary Artery Disease
A heart specialist doctor, or cardiologist, usually diagnoses CAD and determines the extent of the disease, if present, the ability of the heart to function normally, and the optimal form of treatment for the patient. Diagnostic methods include the following:
• Compiling the patient’s medical history, and assessing risk factors
• Performing a physical exam
• Performing diagnostic tests
• Electrocardiogram (ECG or EKG)
A baseline electrocardiogram (ECG or EKG) is performed to record electrical signals as they travel through the heart while the patient sits quietly. An EKG may show reveal evidence of a previous heart attack or a heart attack in progress. An exercise EKG, or stress test, is conducted to determine how the heart responds to increasing exercise. Both tests are used to determine if the heart is not working properly, usually due a lack of oxygen. A holter monitor may be used to test for other abnormalities that show insufficient blood flow to the heart. During this test the patient wears a portable ECG monitor for 24 hours while he or she is doing normal activities.
• Stress test
Basic stress tests include monitoring the electrical activity of the heart while the patient is walking on a treadmill or riding a stationary bike during an EKG. Other stress tests may be performed, if needed.
• Echocardiogram (Echocardiography)
An echocardiogram utilizes sound waves to produce images of the heart to determine if all parts of the heart wall functioning normally in the pumping blood. Sections of heart muscle that move weakly may have been damaged during a heart attack or may be receiving inadequate oxygen. These abnormalities can be detected on an echocardiogram and indicate the presence of coronary artery disease or various other conditions.
• Exercise Stress Tests
• Exercise Thallium Test (Nuclear Stress Rest)
In an exercise thallium test, trace amounts of a radioactive substance such as thallium or a compound known as sestamibi (Cardiolite) are first injected into the bloodstream. While the patient exercises, special cameras detect areas in the heart receiving less blood flow as the blood moves through the arteries. This test not only produces ECG recordings, but also provides images of any damaged or destroyed heart muscle, or of serious narrowing in an artery. For patients who cannot take an exercise test, medications may be given to patients to speed up heartbeat as if the patient were exercising.
• Cardiac catheterization (angiogram).
An angiogram is an x-ray “movie” of heart activity and blood flow through the valves and arteries of the heart. A special dye is first injected into the arteries of the heart to visualize blood flow through the heart. A long, thin, flexible tube (catheter) threaded through an artery, generally in the leg, is inserted to the arteries in the heart. This procedure, called cardiac catheterization, allows the dye to outline narrow and obstructed areas on the X-ray images. If a blockage observed on the X-ray images warrants treatment, then a balloon may be pushed through the catheter and inflated to dilate the blocked blood vessel and improve the blood flow in the coronary arteries. A mesh tube (stent) can then be inserted to keep the dilated artery open.
• CT (Computerized Tomography) Scans
Computerized tomography (CT) technologies, including electron beam computerized tomography (EBCT) or a CT coronary angiogram, are used to visualize the arteries. EBCT, known as an ultrafast CT scan, can detect calcium within plaques that have coronary arteries. A significant amount of calcium may indicate that coronary artery disease is present. In a CT coronary angiogram, a contrast dye is injected intravenously during a CT scan to produce images of the coronary arteries.
• Magnetic Resonance Angiography (MRA)
This procedure combines magnetic resonance imaging (MRI) technology with injection contrast dye to observe areas of narrowing or obstruction. However the outlines of blocked areas may be less clear than in other diagnostic methods.
• Positron emission tomography (PET) scanning
In this advanced nuclear imaging procedure, radioactive tracers (radionuclides) are injected into the blood stream. A PET scan of the coronary arteries shows if the heart is receiving insufficient blood resulting from narrowed arteries or if there are dead cells (scars) from a previous heart attack. The tracers used for PET scans are used to detect injured but still living, or viable, heart muscle that can possibly be saved if adequate blood flow is restored. A PET scan may indicate if the patient is likely to improve from a percutaneous Interventions procedure or surgery to restore blood flow.
Treatments
After a cardiac catheterization has been performed, the 3 most common treatment approaches are lifestyle changes to reduce risk factors, medical therapy, including medications and/or a surgical procedure, and having regular checkups with the cardiologist.
Lifestyle Modification
Patients with diagnosed coronary artery disease should make lifestyle changes to the risk of future cardiovascular events. The main changes include:
• Quit smoking
• Exercise regularly and stay physically active
• Lose excess weight
• Maintain a healthy weight
• Avoid high-cholesterol foods
• Eat a low-fat, low-salt diet that rich in fruits, vegetables and whole grains
• If diabetic, keep blood sugar under control if you have diabetes
• Reduce and manage stress
Medications
Medications may be needed if coronary artery disease cannot be controlled by lifestyle changes. Specific drugs are prescribed, depending on the patient and the extent of the disease.
Blood Thinners (Antiplatelet Therapy)
Antiplatelet therapy is used to treat angina because it reduces the risk of blood clots forming at the sites of the obstruction. Blood thinners can decrease the risk of a blood clot forming which may help prevent obstruction of the coronary arteries
Aspirin
Some patients are advised to take aspirin, the mainstay of antiplatelet therapy for coronary artery disease, or another blood thinner daily to reduce the tendency of the blood to clot. Aspirin may help prevent both blockages of the coronary arteries. In patients who have had a heart attack, aspirin can reduce the risk for future attacks. Patients who have a bleeding disorder or are already taking another blood thinner should check with their doctor before taking aspirin.
Anti-anginal Agents
Beta-blockers are used as first-line therapy for the management of stable angina in all patients with established coronary artery disease. Patients who may have vasospastic angina (chest pain caused by spasm of one of the coronary arteries) should first be treated with a calcium channel blocker or a long-acting nitrate.
Nitroglycerin (Nitro)
Nitroglycerin can control chest pain by dilating the arteries, decreasing the heart’s demand for blood, and improving blood flow to the heart. Nitroglycerin is given in the form of pills, a skin patch, an ointment, or a spray. Nitrates improve exercise tolerance and extend the time to onset of chest pain in patients with angina caused by exertion. All patients who have a history of angina should carry sublingual nitroglycerin. However, nitrates should not be used by patients who have severe aortic stenosis or hypertrophic cardiomyopathy as these drugs may worsen symptoms.
Beta-blockers
Beta-blockers slow the heart rate and reduce blood pressure, which in turn decreases the heart’s demand for oxygen. Beta-blockers inhibit the chemical or hormonal messages sent to the heart, particularly signals for the heart to beat harder when a person is under physical or emotional stress. By blocking the effect of these signals on the heart, beta-blockers decrease the amount of oxygen needed by the heart. Beta blockers also reduce the risk of future heart attacks in patients who have had them.
Calcium channel blockers
Calcium channel blockers relax the smooth muscle muscles surrounding the coronary arteries and cause the vessels to open. These drugs reduce the oxygen demand of the heart, thereby increasing blood flow to the heart and also controlling high blood pressure.
Angiotensin-converting enzyme (ACE) inhibitors and angiotensin II receptor blockers (ARBs)
ACE inhibitors and angiotensin II receptor blockers are similar medications that decrease blood pressure and may help to prevent the progression of coronary artery disease. ACE inhibitors also decrease the risk of future attacks in patients who have had a heart attack.
Percutaneous Interventions and Surgery
Because medications cannot open obstructed arteries, a severely narrowed coronary artery may require more aggressive treatment options to reduce the risk of a heart attack. These options include surgeries and other procedures used to restore blood flow in patients that do not respond favorably to medications. The main non-pharmacologic, or non-drug, procedures are percutaneous interventions (transcatheter interventions) and coronary artery bypass surgery. The therapeutic option depends on the extent or blood vessel narrowing, the number of arteries affected, the location of the narrowing, the amount of heart muscle at risk, and individual patient factors such as age and overall health.
Percutaneous Interventions
Balloon angioplasty and stent placement (percutaneous coronary revascularization)
Angioplasty is also called percutaneous transluminal coronary angioplasty (PTCA). In this procedure, the cardiologist inserts a long, thin tube (catheter) into the narrowed section of the artery. A wire with a deflated balloon is passed through the catheter to the constricted area. The balloon is then inflated, forcing the fatty deposits against the artery walls. A stent is often left in the artery to help keep the artery dilated. Some newer coated stents or drug-eluting stents slowly release medication to help ensure that the artery remains open.
The hospital stay and recovery time for angioplasty is shorter than for coronary bypass surgery. However, nearly 35% of patients who undergo angioplasty are at risk for restenosis, or additional blockages, in the treated area. Restenosis usually occurs within 6 months after angioplasty.
Percutaneous coronary intervention helps to reduce the pain from angina more effectively than medications. However, percutaneous coronary intervention does not increase survival more than do drugs. Aggressive lipid-lowering therapy may be just as effective as percutaneous coronary intervention plus standard medical care for preventing fatal obstruction or a decrease in blood flow to the heart.
Percutaneous transmyocardial revascularization (PTMR)
In percutaneous transmyocardial revascularization, a catheter is inserted into an artery in the leg that leads to the heart. A laser is used to create tiny channels in the lower left chamber (left ventricle) in order to increase blood flow within the heart. The holes are utilized and become channels that allow blood to flow to oxygen-deprived regions of the heart. This procedure appears to trigger the formation of new vessels that can help to decrease the pain of angina. TMLR is less invasive than open heart procedures. It is currently used on patients who have had poor outcomes from treatments such as medications, angioplasty, or coronary artery bypass surgery.
Coronary artery bypass surgery
Coronary artery bypass surgery is an open-heart surgical procedure usually reserved for patients with multiple narrowed coronary arteries. A blood vessel from another part of the body is used to create a graft in order to bypass obstructed coronary arteries. The bypass allows blood to flow around the obstructed or narrowed coronary artery. Because this procedure requires open-heart surgery, it is generally indicated for patients with multiple narrowed coronary arteries.
Minimally invasive coronary artery bypass
This procedure is less invasive than conventional bypass surgery technique. It is appropriate for patients who have a smaller degree of obstruction and a low risk of complications.
Experimental and Innovative Treatment Options
Angiogenesis
In angiogenesis, substances such as stem cells and other genetic material are injected through the vein or directly into damaged heart tissue to trigger the growth of new blood vessels to bypass the clogged ones.
EECP (Enhanced External Counterpulsation)
EECP is a nonsurgical treatment used in patients with chronic angina who have not improved with nitrate medications or who cannot undergo standard surgeries and procedures for coronary artery disease. EECP is an outpatient procedure that increases blood flow to the heart by compressing blood vessels in the lower extremities. Treatment cuffs are placed on the legs which inflate and deflate in order to control the blood supply.
For optimum ways to reduce the risk of coronary artery disease, see your physician for regular check-ups and make lifestyle changes. [LINK]
References
WebMD.com
National Heart Institute
Mayo Clinic
Medline Plus
American Heart Association
Wikipedia.com
National Heart Lung and Blood Institute
Medical News Today
Texas Heart Institute Heart Information Center
Cleveland Clinic





